1st May 2026
Choledochal Cysts: A Surgeon’s Guide to Diagnosis, Treatment and Long-Term Care
Choledochal Cysts: A Surgeon’s Guide to Diagnosis, Treatment and Long-Term Care
By Dr. Appou Tamijmarane, MS, FRCS (Edinburgh, Glasgow & Intercollegiate)
Consultant General, Hepatobiliary-Pancreatic and Upper GI Surgeon — Fakeeh University Hospital, Dubai Silicon Oasis
Reading time: 9 minutes
Quick answer for patients in a hurry
A choledochal cyst is a rare congenital condition where part of your bile duct balloons outwards forming a cystic dilatation. It develops before you are born and not because of anything you ate, drank, or did. Around 85% of people with choledochal cysts have no symptoms at all and are diagnosed incidentally on a scan done for another reason. Once diagnosed, the gold-standard treatment is complete surgical removal of the affected duct followed by reconstruction (Roux-en-Y hepaticojejunostomy), because over time these cysts carry a small but real risk of turning into bile duct cancer.
In my 36 years of surgery, 19 of them as a Consultant in the NHS in the UK and now at
Fakeeh University Hospital in Dubai, I have looked after many patients with this condition. The reassuring news is that with timely diagnosis and the right operation, outcomes are very good and most patients go on to live full, healthy lives.
What exactly is a choledochal cyst?
When patients first hear the term in my clinic, I usually start with this: a choledochal cyst is essentially a part of your bile duct that has “ballooned” out forming a localised dilatation in the tube that carries bile from your liver to your small intestine.
The cyst can develop anywhere along that duct system, from within the liver, down the length of the duct to where it joins the duodenum (the first part of the small intestine). Where exactly the dilatation sits is what defines the type of cyst, and this matters enormously for treatment, which I’ll come back to.
A few important facts to settle the anxiety this diagnosis often creates:
–
It’s congenital. This means you were born with it. The cyst formed while you were a foetus, due to a combination of genetics and the way the tissues around your bile duct developed in the womb.
–
It’s not your fault. I cannot stress this enough. Choledochal cysts are not caused by food, alcohol, smoking, stress, or any environmental factor. Just as everyone has a slightly different nose shape, everyone has small differences in the architecture of their internal organs. A choledochal cyst is one such variation.
–
It’s rare. Choledochal cysts are uncommon worldwide, though they are reported more frequently in East Asian populations.
–
Most people have no symptoms. Around 85% of patients I see with choledochal cysts feel perfectly well. The cyst is picked up incidentally, typically on an ultrasound or MRI ordered for an unrelated reason such as gallstones, a routine health check, or vague abdominal discomfort.
For a comprehensive medical reference, the StatPearls /
NCBI clinical overview of choledochal cysts is an excellent starting point. For a high-quality patient-friendly resource,
the Mayo Clinic also publishes information on bile duct conditions worth reading.
How does a choledochal cyst actually present?
This is one of the most common questions I’m asked, and the honest answer is that the symptoms, when they appear at all, can mimic many other, more common conditions. That’s why an experienced eye matters.
The classic triad
In around 15% of patients, three symptoms appear together, what we call the **classic triad**:
- Right upper abdominal pain
- Jaundice: a yellow tinge to the skin and the whites of the eyes
- A palpable mass in the right upper part of the abdomen
In the real world, very few adult patients present with all three together. That picture is much more common in children. In adult practice, by far the most frequent presenting symptom is
persistent or intermittent pain in the right upper quadrant of the abdomen.
What I look out for that less experienced clinicians sometimes miss
Right upper abdominal pain in an adult is most often blamed on gallstones, indigestion, or muscular pain and most of the time, that’s correct. But when I see a patient, whose pain doesn’t quite fit, especially someone with:
- Recurrent episodes that don’t behave like classical biliary colic
- Mildly abnormal liver enzymes that no one has investigated
- Episodes of fever and pain together (suggesting cholangitis; a bile duct infection)
- A history of unexplained pancreatitis
- A scan that mentions “ductal dilatation” but no clear cause
…I keep choledochal cyst on my differential. The clue is often subtle. Patients themselves frequently say something like
“the pain just doesn’t feel like normal indigestion” and they are usually right.
Why early investigation matters
The reason I push for full investigation rather than reassurance alone is that, untreated, choledochal cysts can lead to:
–
Cholangitis: repeated bile duct infections
–
Pancreatitis: inflammation of the pancreas
–
Bile duct stones that block the duct
–
Progressive liver damage over years
–
Cholangiocarcinoma: bile duct cancer which is the most serious long-term concern
The cancer risk is small in any one year, but it accumulates over a lifetime. That’s why we don’t simply watch and wait, even when patients feel well.
A patient story that taught me a lasting lesson
Illness almost never arrives in a “suitable window” in your life. I remember one patient very fondly, she presented with jaundice and was found to have a choledochal cyst complicated by multiple stones in the bile duct. The corrective operation is major surgery and, even in a fit and healthy patient, carries a very small risk of death.
She was, at the time, breastfeeding a six-month-old baby. She wanted to continue breastfeeding until her child was two. After a long and careful conversation, she chose to delay the surgery. With close management of her symptoms and her bile duct stones, she came through her acute crisis. She was able to continue breastfeeding her baby. She is alive and well today, living happily with her family.
What that case taught me is twofold. First, the right time for surgery is rarely just a clinical question: it is a life question, and a good surgeon respects that. Second, for patients whose symptoms come and go, life takes over once the pain settles, and follow-up gets pushed to the back of the diary. For most that’s manageable. For a small number, that delay matters. Early investigation gives us the widest range of treatment choices and the best surgical outcomes.
How is a choledochal cyst diagnosed?
In my own clinic, the diagnostic pathway is structured and methodical. Here’s exactly how I work through it.
Step 1 Blood tests
I start with
liver function tests and inflammatory markers. If the liver enzymes (ALT, AST, ALP, GGT, bilirubin) are outside the normal range, that justifies further imaging.
Step 2 Ultrasound scan
This is the
first-line imaging investigation. It’s quick, safe, involves no radiation, and is excellent at identifying bile duct dilatation. If the ultrasound suggests a cyst or any abnormality of the duct, we move on to more detailed imaging.
Step 3 MRCP (Magnetic Resonance Cholangiopancreatography)
This is the
investigation of choice for choledochal cysts. MRCP is a specialised MRI scan that maps out, in fine detail, the soft tissues of the liver, gallbladder, bile ducts, and pancreas. It tells us exactly where the cyst is, how big it is, whether other parts of the biliary tree are involved, and whether there are stones inside. Crucially, MRCP is non-invasive and there’s no radiation exposure involved.
Step 4 CT scan (when needed)
If imaging raises concern about a mass or possible cancer within or alongside the cyst, a
CT scan gives us a highly detailed picture of the surrounding structures and helps with surgical planning.
Step 5 — ERCP (only when therapeutic intervention is needed)
ERCP or Endoscopic Retrograde Cholangiopancreatography, combines an endoscopic camera passed through the mouth with X-ray imaging. It’s an invasive procedure, so I reserve it for situations where I need to do something, typically remove stones from the duct, place a stent, or take a tissue sample. In the modern diagnostic pathway, MRCP has largely replaced ERCP as a purely diagnostic test.
The Todani classification explained for patients
When you read your scan report, you will probably see a phrase like “
Type I choledochal cyst on the Todani classification.” This sounds intimidating, but the idea is simple.
Todani is a system that names the cyst based on where in the biliary tree it sits. That location, in turn, dictates the surgical approach.
Here’s the simplest way I explain it to my patients:
- Type I – A cyst on the bile duct outside the liver. This is by far the most common form, accounting for 50–80% of all choledochal cysts.
- Type II – A small “side pouch” off the bile duct, like a diverticulum. Rare (around 3%).
- Type III – A cyst at the very end of the bile duct, where it pokes into the wall of the duodenum (called a choledochocele). Around 4% of cases.
- Type IV – Multiple cysts. Type IVa involves cysts both inside and outside the liver. Type IVb involves multiple cysts outside the liver only. Together, Type IV accounts for around 12–35% of cases, the second most common pattern.
- Type V – Multiple cysts confined to the bile ducts inside the liver. This is also known as Caroli disease.
The diagram below shows each of these types along the biliary tree at a glance.
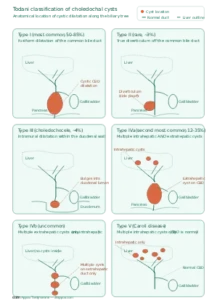
The reason this classification matters is that the surgical plan changes significantly between types. Type I and Type IV (the two most common adult presentations) are managed with complete cyst excision and biliary reconstruction. Type II is a simpler diverticulectomy. Type III is sometimes managed endoscopically. Type V (Caroli disease) may need a partial liver resection or, in advanced bilateral disease, even a liver transplant.
Why surgery — and why complete excision?
Many patients ask me, “
If my cyst is small and I have no symptoms, why operate at all?” It’s a fair question and I want to answer it directly.
There is no medical treatment for a choledochal cyst. No tablet, diet, or lifestyle change will make it go away. Drainage alone, or partial removal, leaves residual abnormal tissue behind and abnormal bile duct tissue is the tissue that, over years, can develop into cancer.
The aim of the operation is therefore twofold:
- Remove the abnormal duct entirely: including the cyst, the gallbladder, and any affected portion of the duct, ideally as a single, intact piece.
- Reconstruct the bile flow so bile can drain freely from the liver into the intestine again.
The Roux-en-Y hepaticojejunostomy
The gold-standard reconstruction is called a
Roux-en-Y hepaticojejunostomy. The name sounds complicated; the principle is elegant.
After we have removed the entire affected bile duct as a single piece (so that no bile or stones spill into the abdomen during the operation), we take a loop of small bowel and bring it up to where the healthy bile duct emerges from the liver. We then
connect the healthy duct directly to that loop of small bowel, creating a clean, stone-free, cancer-resistant new pathway for bile to flow from your liver into your intestine.
Two specific reasons I prefer this reconstruction:
- Oncological safety by removing the entire abnormal duct, we substantially reduce (though never eliminate) the long-term cancer risk.
- Mechanical longevity the Roux-en-Y configuration discourages food contents from refluxing back up into the bile duct, which reduces the risk of recurrent infections.
For Type V (Caroli) disease, where the cysts are entirely within the liver, treatment may require
liver resection of the affected portion. In severe, diffuse cases,
liver transplantation is considered.
Open, laparoscopic, or robotic surgery, which approach is right?
Patients often ask whether their cyst can be removed through “keyhole” surgery. The honest, surgeon-to-patient answer is this:
A complete cyst excision requires very careful dissection of the bile duct away from the major blood vessels behind it (the portal vein and hepatic artery), as well as careful handling of the pancreas where the lower end of the duct sits. The plane of dissection has to be perfect, being too aggressive risks injuring blood vessels or too cautious risks leaving abnormal tissue behind.
For this reason,
open surgery still gives the surgeon the optimal views and access for the most reliable, safest, and most complete excision in adult patients. That is currently my preferred approach for the majority of choledochal cyst operations.
That said,
laparoscopic and robotic techniques are evolving rapidly. In carefully selected patients, typically those with simpler Type I anatomy, no previous inflammation, and no concern about cancer, minimally invasive approaches are becoming a credible option. As technology continues to advance and surgeon experience grows, I expect this trend to continue.
The bottom line: the
best operation is the one that removes all the abnormal tissue safely. That is what I will plan for you, and we will discuss the trade-offs of each approach openly before any decision is made.
What about recovery, follow-up, and long-term cancer risk?
After surgery, you’ll typically spend a few days in hospital. Recovery from open Roux-en-Y reconstruction is usually 6–8 weeks back to normal activity, with most patients eating and walking comfortably within the first week.
Why we follow you up for life
Even with the most meticulous excision, a small portion of the bile duct usually has to be left behind at the lower end where the duct meets the pancreas, and at the top end where the duct enters the liver. Both of those segments retain a small, residual long-term cancer risk.
For this reason, I personally recommend
annual MRCP imaging after this surgery, indefinitely. This is a non-invasive scan, and it allows us to detect any change at the earliest possible stage. Most of my post-operative patients live entirely normal lives between these annual scans.
Symptoms to watch for after surgery
Please attend an emergency department urgently if, at any point after your surgery, you develop:
- New jaundice yellowing of the skin or eyes
- Fever with abdominal pain possible cholangitis
- Persistent vomiting or inability to keep food down
- Significant unexplained weight loss
- A return of the pain pattern that originally led to your diagnosis
These symptoms don’t always mean something serious, but they always deserve to be checked.
When should you see a specialist?
You should ask for an HPB (hepatobiliary) surgical opinion if:
- A scan has reported “bile duct dilatation” or “possible choledochal cyst”
- You have had recurrent right upper abdominal pain that has never been fully explained
- You have unexplained jaundice or repeatedly abnormal liver function tests
- You have had unexplained pancreatitis, particularly more than once
- You have a known choledochal cyst and you have not had recent surveillance imaging
You can also read my related guides on
liver cysts and
malignant liver tumours for context on related biliary conditions.
A final word
If you have just been told you have a choledochal cyst, I want to leave you with this. It is a rare condition, but it is a
known condition with a
clearly defined treatment pathway and
very good long-term outcomes when managed by an experienced HPB surgeon. The diagnosis can be unsettling, especially when you read about cancer risk, but the entire purpose of the surgery I have described is precisely to address that risk proactively, before it becomes a problem.
Take your time. Ask questions. Bring a family member to your consultation. And get a second opinion if it gives you peace of mind – I encourage that for every patient considering major surgery.
If you would like to discuss your scan, your symptoms, or your treatment options, my team and I would be very glad to help.
Book a consultation with Dr. Appou Tamijmarane
📍 Fakeeh University Hospital, Dubai Silicon Oasis
📞 +971 503 567 569 (tel:+971503567569)
✉️
info@drappou.com
💬
Chat on WhatsApp
🗓️
Book an appointment online
Further reading from trusted medical sources
–
StatPearls / NCBI Bookshelf – Choledochal Cyst (clinical overview)
–
Mayo Clinic – Bile duct conditions and biliary surgery
Medical disclaimer: This article is for general educational purposes and is not a substitute for individual medical advice, diagnosis, or treatment. If you are concerned about your symptoms or your diagnosis, please consult a qualified healthcare professional. Dr. Appou Tamijmarane is licensed by the Dubai Health Authority and practises at Fakeeh University Hospital, Dubai Silicon Oasis.
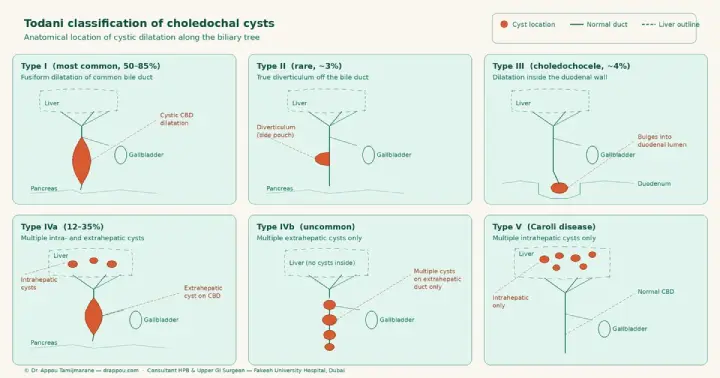
 The reason this classification matters is that the surgical plan changes significantly between types. Type I and Type IV (the two most common adult presentations) are managed with complete cyst excision and biliary reconstruction. Type II is a simpler diverticulectomy. Type III is sometimes managed endoscopically. Type V (Caroli disease) may need a partial liver resection or, in advanced bilateral disease, even a liver transplant.
The reason this classification matters is that the surgical plan changes significantly between types. Type I and Type IV (the two most common adult presentations) are managed with complete cyst excision and biliary reconstruction. Type II is a simpler diverticulectomy. Type III is sometimes managed endoscopically. Type V (Caroli disease) may need a partial liver resection or, in advanced bilateral disease, even a liver transplant.